The risk ratio (RR) and 95% confidence interval (CI) were determined. The outcomes of the present analysis were as follows: all-cause mortality, cardiovascular mortality, ischemic stroke, heart failure (HF) hospitalization, nights spent in hospital per year, acute coronary syndrome, major bleeding, and cardiac arrest/ventricular arrhythmia.ĭichotomous variables were investigated using the Mantel-Haenszel method. The following information was gathered from eligible studies: (1) design of the research (2) primary/secondary outcome (3) mean follow-up time and baseline characteristics and (4) anticoagulation therapy, rate, and rhythm protocols. The risk of bias was assessed using the Cochrane collaboration tool for RCTs and using the Newcastle-Ottawa scale for non-randomized clinical studies. Disagreements were addressed by consensus and, if needed, the consulting of a third reviewer. Two reviewers separately evaluated article titles and abstracts to exclude papers that were not relevant. Reviews, case studies, conference papers, comments, and animal trials were all omitted from the study. 
All studies were restricted to those including human subjects who were at least 18 years old. rate control (2) based on “Early Treatment of Atrial Fibrillation for Stroke Prevention Trial” (EAST-AFNET 4) study, patients were enrolled within 1 year after the first diagnosis of AF (early AF) ( 10) (3) the studies’ follow-up time was at least 1 year and (4) the goal of the study was to examine the effect and prognosis of AF treated with early rhythm vs. The following criteria were used to choose articles: (1) observational studies or RCTs that included patients with AF based on early rhythm control vs. To determine whether early rhythm control is better than rate control in patients with AF, we performed a systematic review and meta-analysis. 
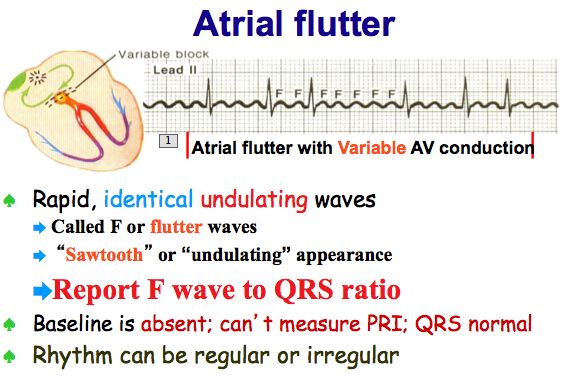
Several studies have recently shown that the incidence of adverse cardiovascular outcomes was reduced by early rhythm control compared with rate control ( 10– 17). However, the treatment of AF has changed dramatically since the above RCTs were published. No significant difference in all-cause mortality, cardiovascular mortality, and other related morbidities was found between rhythm control and rate control in the meta-analyses of the above studies included ( 8, 9). The choice of rhythm or rate control in current guidelines relies on several randomized controlled studies (RCTs) ( 5– 7). rate control strategies have differing effects on mortality and morbidity for AF. It has been argued for a long time whether rhythm vs. Rhythm control refers to the use of antiarrhythmic drugs, cardioversion, and AF ablation to try to restore and maintain sinus rhythm. Rate control is part of AF management and can adequately improve related symptoms. The current two essential aims of AF clinical care are (1) thromboembolism prophylaxis with anticoagulation and (2) maintenance of an appropriate heart rate or sinus rhythm by medications or interventional procedures ( 4). 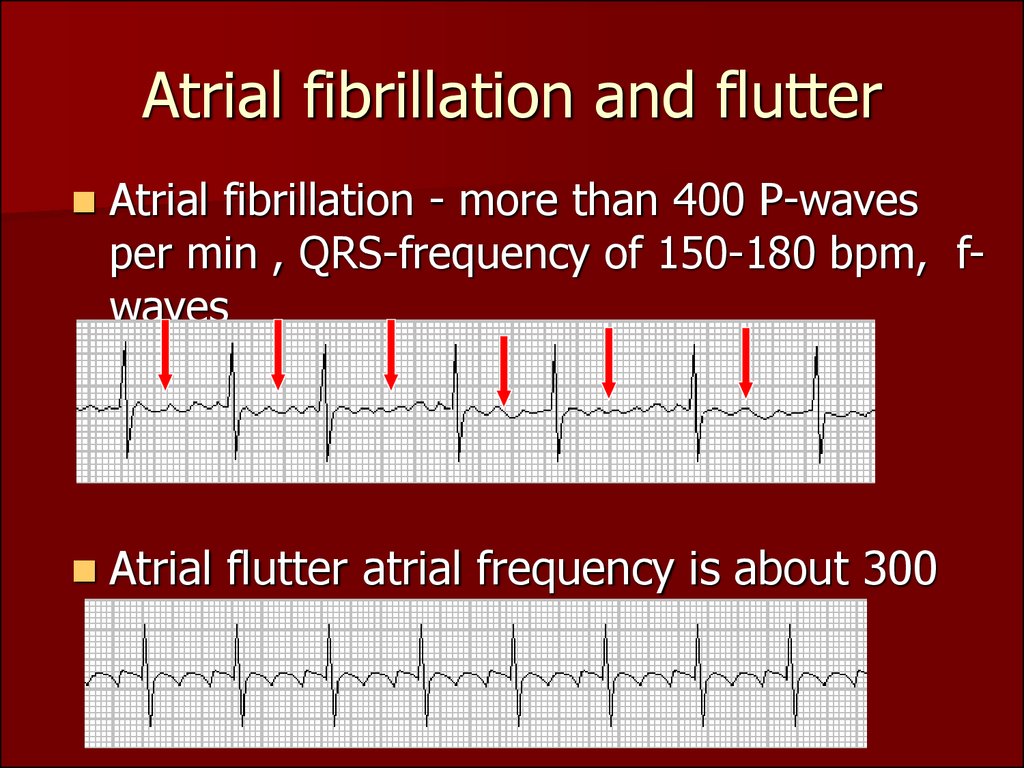
Atrial fibrillation (AF) is a kind of cardiovascular disease that affects millions of people throughout the world and is associated with an increased risk of mortality and morbidity, with a fivefold increased risk of stroke ( 1– 3). 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
